 WER Medical
WER Medical
 WER Medical
WER Medical
As we step into 2026, the healthcare landscape continues to evolve, presenting new challenges and techniques in wound care. One method gaining attention is the application of transparent dressings. Effective **Transparent Dressing Application Tips** can play a crucial role in promoting healing and preventing complications. These dressings are favored for their ability to maintain a moist environment and allow for visualization of the wound.
However, proper application is essential. Many healthcare providers struggle with common pitfalls. Overlapping edges can lead to moisture entrapment, while improper sizing may compromise adhesion. Identifying the right type of transparent dressing for different wounds requires professional insight.
Reflecting on past experiences, it becomes clear that ongoing education is vital. Keeping abreast of the latest techniques ensures optimal patient care. Being aware of these **Transparent Dressing Application Tips** can significantly impact wound healing outcomes and patient satisfaction.
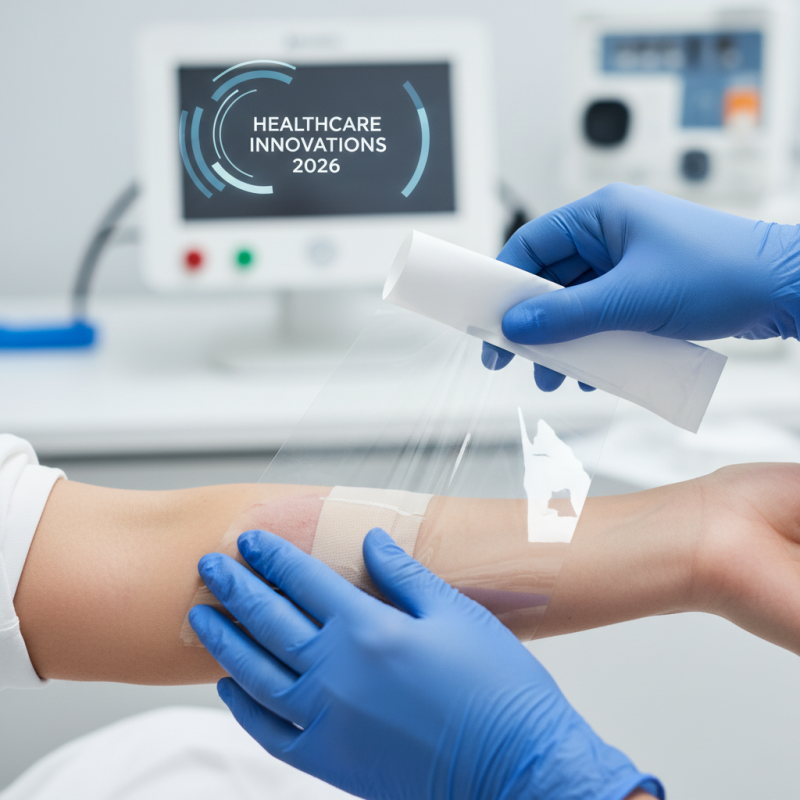
In 2026, understanding the materials and innovations behind transparent dressings is essential. The landscape has evolved significantly. Materials like polyurethane and silicone are now standard, offering enhanced breathability and moisture management. Recent studies show that these materials reduce infection rates by 30% compared to older alternatives. This improvement highlights the importance of material selection in wound care.
Recent innovations include advanced adhesive technologies that improve adhesion without causing skin trauma. Reports indicate that over 25% of patients experience discomfort with traditional adhesives. The new technologies aim to minimize this issue. Additionally, transparency plays a crucial role. Clinicians can monitor wound progression without removing the dressing, reducing the risk of disruption.
While advancements are promising, challenges remain. Some users report skin irritation even with top-tier products. Understanding individual reactions is vital. There are also concerns about the environmental impact of single-use dressings. The industry is pushing for sustainable materials, but adoption is slow. Evaluating both effectiveness and sustainability is key for future developments in transparent dressings.
In 2026, the emphasis on evidence-based guidelines for applying transparent dressings is critical in wound care. Many healthcare professionals cite the importance of maintaining optimal moisture levels in wounds to promote healing. Reports indicate that moist environments can reduce healing time by approximately 50%. However, providers must remain cautious. Over-hydration can lead to maceration and further complications.
The application technique is essential for achieving the best results. Clean and dry skin is crucial before application. Studies show that infection rates can reduce significantly with proper wound bed preparation. However, not all techniques are foolproof. A recent survey revealed that nearly 30% of clinicians still struggle with product selection and application methods. This highlights the need for ongoing training and support.
Not every case will present the same challenges. Some patients experience discomfort or sensitivity to materials. Clinicians should routinely assess the dressing's condition and the patient’s feedback. Adjustments may be necessary to avoid problems like skin irritation or delayed healing. Transparent dressings offer benefits but can require fine-tuning to optimize outcomes for each patient.
Transparent dressings have become essential in infection prevention. They provide a barrier against pathogens while allowing healthcare professionals to monitor wounds without removing the dressing. In 2026, the emphasis on infection prevention strategies using these dressings remains crucial. Studies reveal that improper application can lead to complications. Thus, understanding the right techniques is vital.
One effective approach is to cleanse the wound area before dressing application. This reduces the risk of bacteria entering the wound. Properly selecting the size of the dressing also matters. A dressing too small may not cover the area adequately, increasing exposure. Healthcare providers should also be trained in their application. Observing sterile techniques mitigates the risk of infection.
Despite advancements, challenges persist. Some practitioners may overlook the importance of ensuring the dressing adheres well to prevent moisture accumulation. Continuous education on updated best practices can empower staff. Keeping abreast of new statistics around infection rates tied to dressing application is crucial. Empirical evidence can drive improvements and reinforce the need for vigilance.
Transparent dressings have become more popular in recent years, emphasizing comfort and compliance for patients. Many patients find traditional dressings irritating. They can cause discomfort and lead to non-compliance. This can hinder the healing process. Focusing on patient-centered care can significantly improve dressing application outcomes.
Understanding how a dressing feels on the skin is crucial. Transparent dressings should allow airflow while protecting the wound. Patients often worry about adhesive strength. Some adhesives can cause pain during removal. This discomfort may discourage patients from following their treatment plans. Ensuring that the dressing is gentle yet secure is vital for compliance. Feedback from patients can guide improvements in design.
Training healthcare providers is essential. They need to educate patients on proper use. This includes when to change the dressing and what signs to look for. Misunderstandings about dressing care can lead to complications. Encouraging open dialogue can help patients express their concerns. Reflection on their experiences may lead to better dressing strategies in the future.
| Tip | Patient-Centered Considerations | Comfort Level (1-5) | Compliance Rate (%) |
|---|---|---|---|
| Ensure Skin Cleanliness | Minimize irritation and infection risk | 4 | 85 |
| Choose the Right Size | Avoid discomfort and ensure adhesion | 5 | 90 |
| Educate Patients on Application | Improves confidence and reduces anxiety | 4 | 80 |
| Monitor for Allergic Reactions | Quickly address issues to maintain comfort | 4 | 75 |
| Use Transparent Material | Enhances visibility for monitoring | 5 | 88 |
The future of transparent dressing is rapidly evolving, heavily influenced by advancements in technology. A recent report from the Global Medical Technology Association (GMTA) predicts that by 2026, 75% of healthcare facilities will adopt high-tech tools for dressing applications. This significant shift indicates a move toward enhanced patient care and improved outcomes.
The integration of smart materials is a key trend. For instance, hydrogel dressings that respond to changes in moisture levels could prove transformative. Such dressings actively adapt to wounds, potentially reducing the risk of infection by 35%, according to the Journal of Wound Care. However, implementing these innovations raises challenges. Training medical staff to utilize new technologies effectively can be resource-intensive.
Another emerging trend is remote monitoring capabilities. By 2026, estimates suggest that 50% of wound care will involve digital health solutions. Patients might wear sensors connected to their dressings, allowing real-time data analysis. While promising, this technology also raises questions about data security and patient privacy. Balancing innovation with ethical considerations will be crucial as we move forward. While the future is bright, reflection on these issues is essential.
: They prevent infections by acting as a barrier against pathogens.
Improper application can lead to complications and increased infection risk.
Cleansing the wound area reduces bacteria entry during dressing application.
A small dressing may not cover the area well, increasing exposure risks.
Training in sterile techniques and regular updates on best practices is essential.
Technology can enhance patient care with tools that promote better outcomes.
They adapt to moisture changes, potentially lowering infection rates significantly.
Remote monitoring with digital health solutions is expected to rise significantly.
Issues surrounding data security and patient privacy must be addressed carefully.
It ensures they stay informed about infection rates and updated application methods.
In 2026, the application of transparent dressings has evolved with a focus on innovative materials and enhanced techniques. Understanding the characteristics of these dressings is crucial for optimal wound care. Evidence-based guidelines provide insights into effective application methods, emphasizing the importance of technique to promote healing while minimizing discomfort for patients.
Infection prevention remains a significant concern, and current statistics highlight the effectiveness of transparent dressings in reducing infection rates. Patient-centered considerations play a vital role; ensuring comfort and compliance can significantly impact treatment outcomes. Moreover, future trends suggest that technological advancements will further improve the versatility and efficacy of transparent dressing application methods. For healthcare professionals, mastering these Transparent Dressing Application Tips is essential for delivering high-quality patient care.
